Heart disease rarely appears suddenly. The body gives signals long before major complications develop. Recognizing these early symptoms can help you seek treatment before damage becomes severe or irreversible.

1. Subtle Chest Discomfort or Pressure
A quiet warning that often gets ignoredMany people expect heart pain to be dramatic, but early heart disease usually starts with a quiet, lingering pressure or heaviness in the chest. It may not feel painful; instead, it can resemble indigestion, tightness, or a dull warmth behind the breastbone. These sensations often appear during activity, emotional stress, or after meals, and they typically calm down with rest. What makes this dangerous is that people dismiss it, assuming it’s acidity or fatigue. In reality, the heart may be receiving less oxygen because the arteries are gradually narrowing. Over time, this restriction worsens and turns into more serious symptoms that could have been prevented if this early sign had been recognized.
When chest sensations are new, occur with exertion or emotional triggers, or are accompanied by jaw or arm discomfort, they warrant clinical attention. A careful history, simple tests such as ECG or stress testing, and, when indicated, coronary imaging can determine whether coronary artery disease is the cause and whether interventions medical or procedural are appropriate to reduce risk and relieve symptoms.

2. Shortness of Breath During Normal Activities
Breathing feels heavier than it used toWhen the heart struggles to pump efficiently, your lungs work harder to compensate. Fluid can start building up in lung tissues, making simple activities like climbing stairs or walking at a normal pace feel exhausting. People often assume they are “out of shape,” but a noticeable decline in stamina especially when your lifestyle hasn’t changed is one of the clearest signs of developing heart issues. The shortness of breath may initially come and go, but it gradually becomes consistent as the heart weakens. Identifying this pattern early can help prevent chronic heart failure in the future.
Clinicians assess breathlessness by asking about onset, triggers, and daily patterns; they may perform lung and heart imaging, measure oxygenation, and use stress testing to check how the heart responds to exertion. Treatment that improves heart function from lifestyle changes and medications to targeted procedures often leads to marked improvements in breathlessness and quality of life.
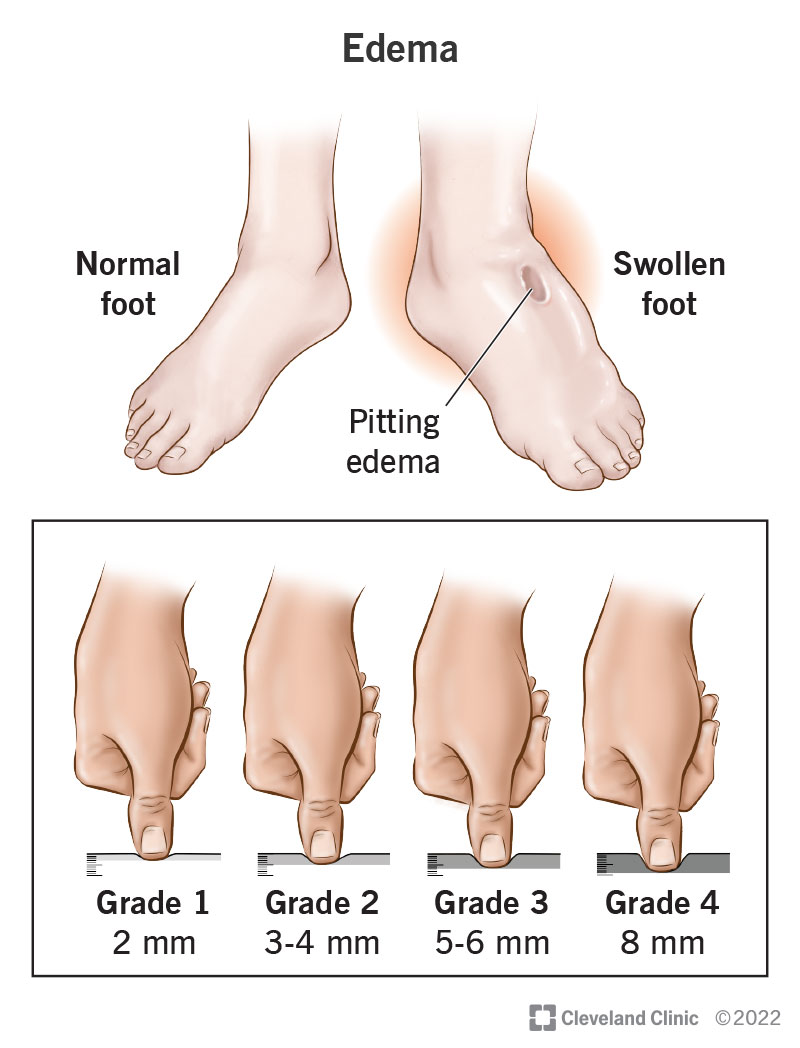
3. Swelling in Legs, Ankles, or Feet
Fluid retention caused by weakened circulationProgressive swelling in the lower limbs is a common and often underappreciated sign that the heart may be struggling. When cardiac output falls, pressure in the venous system rises and fluid gradually moves into the tissues, producing visible puffiness that typically worsens during the day and improves overnight. Initially, swelling may be subtle: a slight tightness in shoes, an indentation after pressing the skin, or a sense of heaviness in the legs. Over weeks, this can become more obvious and persistent.
Because many conditions can cause edema from kidney problems and liver disease to medication side effects and venous insufficiency clinicians look for accompanying cardiac clues such as breathlessness, fatigue, or elevated jugular venous pressure. Early management focuses on reducing contributing factors (salt intake, sedentary behaviour), using measured leg elevation and compression when appropriate, and treating the underlying cardiac dysfunction with medications that support the heart and help mobilize excess fluid. Timely recognition prevents progressive congestion and reduces the risk of hospitalisation.
In practice, documenting daily weight, noting how swelling responds to rest, and sharing this pattern with a clinician enables early intervention. When edema follows a consistent worsening trend despite simple measures, further cardiac evaluation including echocardiography to assess heart function becomes important to tailor therapy effectively.

4. Unexplained Dizziness or Lightheadedness
A sign the brain isn’t receiving enough bloodBrief episodes of dizziness or a feeling of faintness often arise when the brain temporarily receives less blood than it needs. In cardiac terms, this can be caused by a sudden drop in cardiac output, arrhythmias that interrupt effective circulation, or obstructive valve lesions that impede flow. The sensation may be transient and easily dismissed, yet repeated episodes can be an early signal of significant cardiovascular instability.
A clinician will attempt to correlate dizziness with posture changes, timing (e.g., during exertion), medications, or other symptoms such as palpitations or chest discomfort. Investigations may include orthostatic blood pressure testing, ambulatory rhythm monitoring, and echocardiography. Identifying an arrhythmia or structural cause early allows targeted treatments that restore stable circulation and significantly reduce the risk of fainting and injury.
Practical self-care while pursuing medical assessment includes sitting or lying down at the first sign of lightheadedness, staying hydrated, and avoiding sudden posture changes until an underlying cause is clarified and managed.
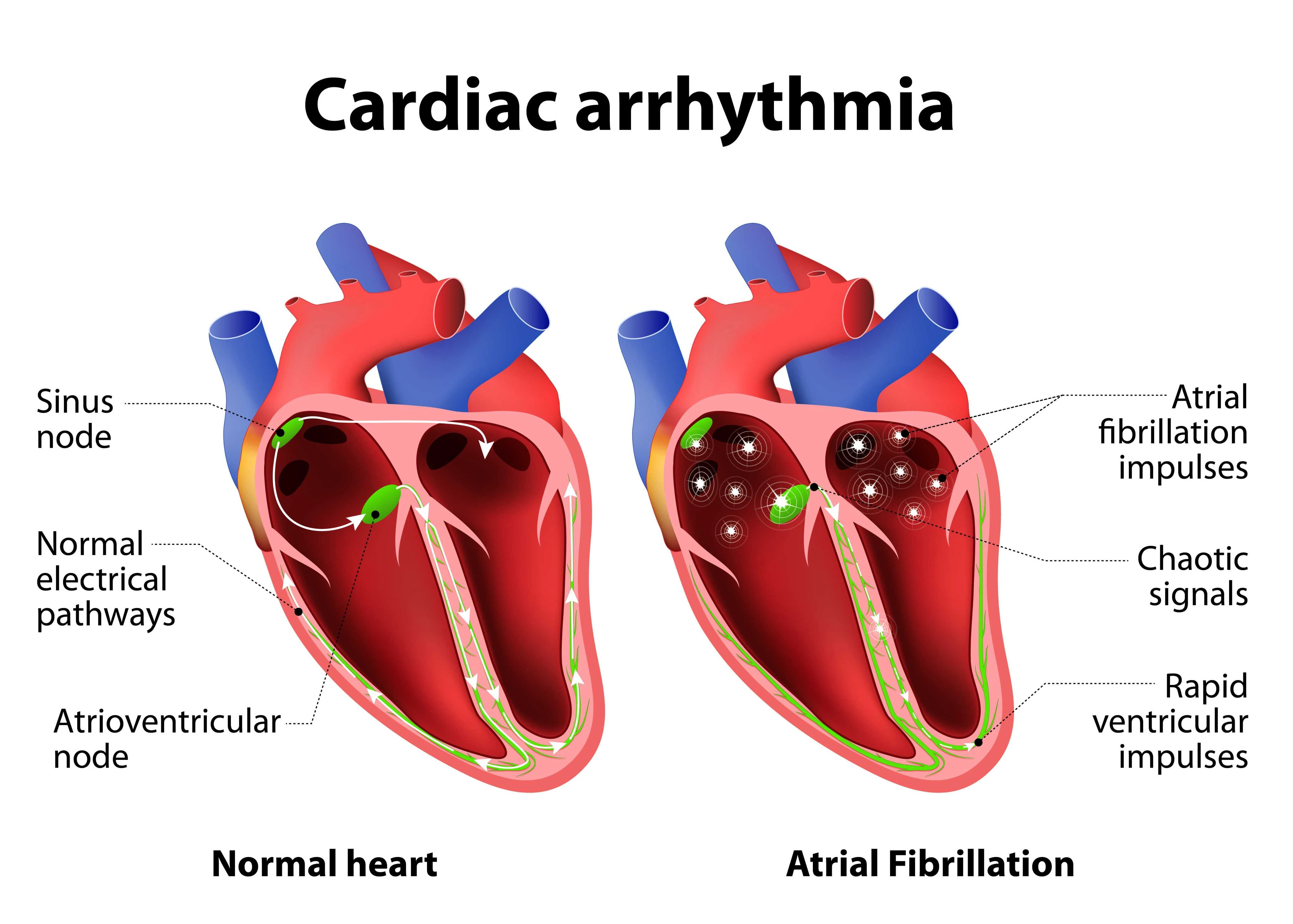
5. Irregular Heartbeats or Fluttering Sensations
Your heart may be signaling electrical instabilityAwareness of an abnormal heartbeat sensations of fluttering, rapid pounding, or recurrent skipped beats can indicate disturbances in the heart’s electrical system. While isolated palpitations can be benign (often triggered by caffeine, stress, or lack of sleep), persistent or recurrent episodes deserve evaluation because certain arrhythmias raise the risk of stroke, heart failure, or sudden syncope.
Clinicians classify palpitations by their pattern, duration, and triggering factors. Diagnostic tools include resting ECG, extended ambulatory monitoring (Holter), and event recorders that capture the rhythm during symptomatic episodes. When an arrhythmia is identified, treatment options vary widely from reassurance and lifestyle modification to medications, catheter ablation, or device therapy and are chosen to reduce symptoms and long-term risks.
Tracking episodes (what you were doing, how long they lasted, and any accompanying signs such as dizziness or chest pressure) can significantly improve diagnostic accuracy and help clinicians select the most effective intervention.

6. Persistent Unusual Fatigue
Your heart works harder than you feelFatigue is one of the most common, yet overlooked, early presentations of heart disease. Unlike ordinary tiredness that improves with rest, cardiac fatigue is persistent and may be accompanied by an inability to perform tasks that were previously routine. The heart’s diminished capacity to meet the body’s oxygen demands forces other systems to compensate, leaving muscles and organs under-perfused and the patient chronically drained.
Women often describe fatigue as their primary and sometimes sole initial symptom of coronary disease. A thorough evaluation examines other potential contributors anemia, thyroid dysfunction, sleep disorders while concurrently assessing cardiac status with imaging and function tests. Importantly, improving cardiac function through treatment and lifestyle change often produces pronounced recovery from this type of fatigue.
Practical steps for patients include keeping a symptom diary, noting activity levels that provoke marked tiredness, and sharing these details with a clinician to facilitate timely testing and interventions.

7. Nausea or Indigestion-Like Sensations
When stomach symptoms are actually cardiacBecause the heart and digestive tract share neural pathways, cardiac ischemia can be misinterpreted as indigestion, upper abdominal discomfort, or nausea. This presentation is particularly common among women and older adults, who may report queasiness or a persistent “indigestion” that is not relieved by antacids. The danger lies in dismissal: recurring or exertion-related gastrointestinal sensations can mask significant heart disease if not evaluated in context.
Clinicians assess timing (for example, whether the symptoms occur with activity), associated features (sweating, breathlessness, lightheadedness), and response to typical gastrointestinal treatments. When cardiac causes are suspected, ECG, enzymes, and imaging may be used to rule out ischemia. Early recognition avoids delays in therapy and reduces the chance of progression to more severe events.
If you experience new or recurrent nausea or unexplained upper abdominal discomfort especially if it occurs with other subtle symptoms seek medical review rather than self-treating repeatedly with over-the-counter remedies.
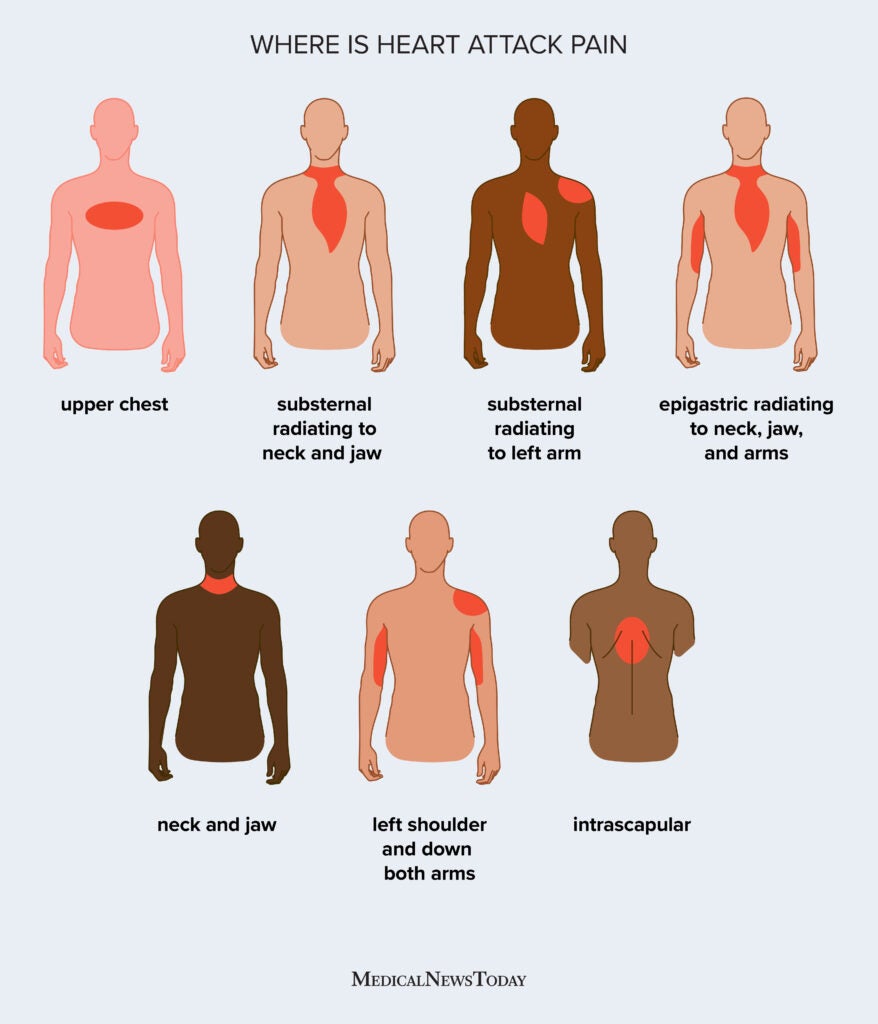
8. Pain Radiating to Jaw, Neck, or Arm
A classic but often misunderstood signalThe heart’s nerve supply overlaps with regions such as the jaw, neck, shoulders, and upper back; as a result, cardiac ischemia can present as pain in these distant sites rather than the chest. This “referred” pain may be mild and intermittent early on, leading patients and clinicians to search for dental, musculoskeletal, or gastrointestinal causes instead of considering cardiac origins.
Recognising the association between exertion and referred pain, and noting accompanying symptoms like breathlessness, diaphoresis, or unusual fatigue, helps clinicians prioritise cardiac investigation. Diagnostic pathways may include ECG, stress testing, and coronary imaging when indicated. Early detection of coronary issues that present atypically improves outcomes and allows timely preventive or corrective measures.
For patients, careful description of the pain’s relationship to activity, duration, and accompanying sensations offers critical clues that expedite correct diagnosis.

9. Difficulty Sleeping or Night Sweats
Your heart may be struggling during restSleep disturbances and night sweats can reflect early cardiac strain. When laying flat increases the heart’s workload or pulmonary congestion, people may awaken gasping, feel unusually sweaty at night, or sleep poorly due to breathlessness. These nocturnal symptoms are often misattributed to anxiety or hormonal changes, but when they coincide with daytime fatigue or reduced exercise tolerance they point toward an underlying cardiovascular problem.
Evaluation often involves assessing sleep quality and looking for obstructive sleep apnea a condition tightly linked with hypertension and heart disease alongside cardiac imaging and functional testing. Treating sleep-related contributors while optimising cardiac therapy often restores sleep quality and reduces cardiovascular risk.
Practical steps include monitoring sleep patterns, avoiding heavy meals and stimulants before bedtime, and discussing persistent night symptoms with a clinician who can coordinate sleep and cardiac evaluations.
10. High Blood Pressure That’s Hard to Control
A major silent driver of long-term damageHypertension is one of the most important and insidious contributors to heart disease. Often symptomless, high blood pressure steadily damages arterial walls, increases the heart’s workload, and leads to muscle thickening and stiffening. When blood pressure remains elevated despite lifestyle measures and first-line medication, it signals that more aggressive control or investigation is needed to prevent longer-term complications such as heart failure, coronary disease, stroke, and kidney damage.
Managing resistant hypertension includes reviewing medication adherence, lifestyle factors, secondary causes (such as sleep apnea or endocrine disorders), and sometimes adding or changing pharmacologic therapies. Early detection and meticulous control of blood pressure reduce structural heart changes and markedly lower long-term cardiovascular risk.
For patients, regular home monitoring, keeping a blood pressure log, and sharing it with their care team, and promptly addressing any readings that remain high helps clinicians tailor therapy effectively and protect heart health over the long term.

Leave a Reply