Explore how artificial intelligence is improving diagnosis accuracy and patient outcomes.

1. Faster, More Accurate Medical Imaging Interpretation
AI as a second pair of eyes for radiology and pathologyMachine learning models trained on thousands of labeled scans now assist radiologists by highlighting suspicious areas, quantifying lesion size, and prioritising urgent cases. In many settings these tools reduce time-to-diagnosis and improve detection of subtle abnormalities that might be missed on a busy worklist.
Importantly, AI does not replace clinical judgement — it augments it. When integrated thoughtfully, automated image analysis improves consistency, reduces variability between readers, and allows clinicians to focus on complex interpretive tasks and patient communication.

2. Clinical Decision Support and Risk Prediction
Predicting deterioration and tailoring interventionsPredictive algorithms analyse electronic health record data to flag patients at high risk for sepsis, readmission, or rapid deterioration. These early warnings give care teams time to intervene, often preventing escalation and shortening hospital stays.
When crafted with transparency and validated locally, these models become practical tools for triage and resource allocation. Ongoing clinician oversight ensures that predictions translate into meaningful, patient-centred action rather than alert fatigue.

3. Remote Monitoring and Continuous Care
Wearables, sensors and AI keep patients connectedWearable devices combined with onboard analytics detect arrhythmias, track activity, and monitor vital signs continuously outside the clinic. AI algorithms can triage this data, sending actionable alerts to clinicians only when patterns suggest real concern, which reduces unnecessary visits and enables timely home-based care.
Remote monitoring improves chronic disease management — for heart failure, diabetes, or COPD — by allowing more granular treatment adjustments and earlier recognition of deterioration, improving outcomes while increasing patient convenience.
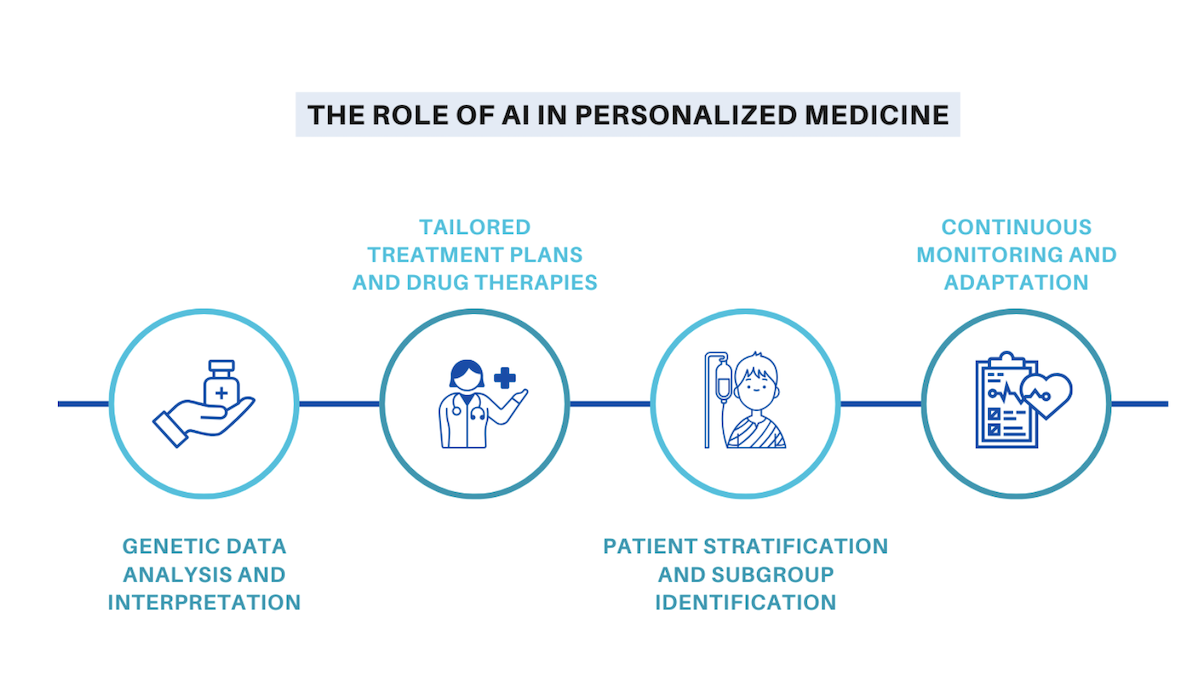
4. Personalised Medicine and Treatment Optimisation
Matching therapies to the individual patientBy integrating genomic, clinical and lifestyle data, AI helps identify which patients will benefit most from particular drugs or dosing strategies. This precision approach reduces trial-and-error prescribing and can minimise adverse effects while improving therapeutic response.
In oncology and rare diseases, model-driven recommendations accelerate selection of targeted agents and trial opportunities, giving clinicians better information when making high-stakes decisions.
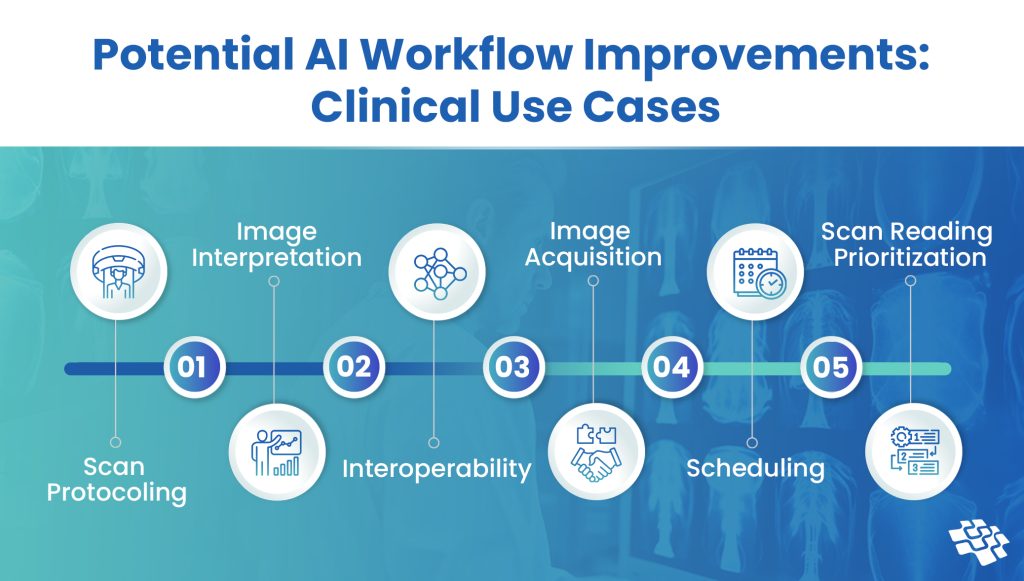
5. Operational Efficiency and Workflow Automation
Reducing administrative burden, freeing clinicians for careNatural-language processing and robotic process automation extract information from notes, automate scheduling, and streamline billing. These efficiencies shrink administrative tasks that consume clinician time, enabling staff to spend more time with patients.
Thoughtful deployment focuses on augmenting human teams rather than replacing them; when workflow tools are well-integrated they reduce errors and speed care delivery without compromising safety.
6. Accelerating Drug Discovery and Clinical Trials
From molecule screening to smarter trial designAI models screen vast chemical libraries and predict candidate molecules with desirable properties, dramatically shortening early-stage discovery timelines. In clinical trials, AI helps identify optimal patient cohorts and predict likely responders, improving trial efficiency and success rates.
These capabilities make it possible to bring promising therapies to patients faster and reduce the cost burden of development, but they still require rigorous experimental validation before clinical use.

7. Data Governance, Privacy and Ethical Use
Balancing innovation with patient rights and safetyAI depends on high-quality data, which raises critical concerns about consent, de-identification, and equitable representation. Poorly governed datasets can reproduce bias, producing worse outcomes for underrepresented groups.
Robust governance frameworks, transparent model reporting, and continuous performance monitoring are essential to ensure systems remain fair, explainable, and aligned with clinical values. Patient trust depends on clear policies and accountable stewardship of sensitive health information.
8. Clinical Validation and Regulatory Pathways
From promising prototype to trusted clinical toolBefore deployment, AI tools require rigorous clinical trials, real-world validation and regulatory review to confirm safety and effectiveness. Validation across diverse populations prevents performance drift and ensures the tool generalises beyond the original development environment.
Regulatory agencies are evolving frameworks for algorithmic medical devices; successful adoption depends on clear evidence of benefit, ongoing post-market surveillance, and mechanisms for updates without compromising patient safety.

9. The Human-AI Partnership and Future Directions
Designing systems that amplify human expertiseThe most successful AI deployments treat clinicians as partners: systems that present clear rationale, surface uncertainty, and integrate seamlessly into clinical workflows earn trust and adoption. Educational programs that train clinicians to interpret and challenge AI output are equally important.
Looking ahead, federated learning, improved model interpretability, and closer patient involvement in design promise safer, more personalised tools. When built responsibly, AI will continue to shift care from reactive to proactive, improving outcomes while preserving human compassion.