Women’s Health: Complete Wellness Guide — Learn about PCOS, menstrual health, fertility care, and essential wellness tips for women of all ages.
Understanding Menstrual Health
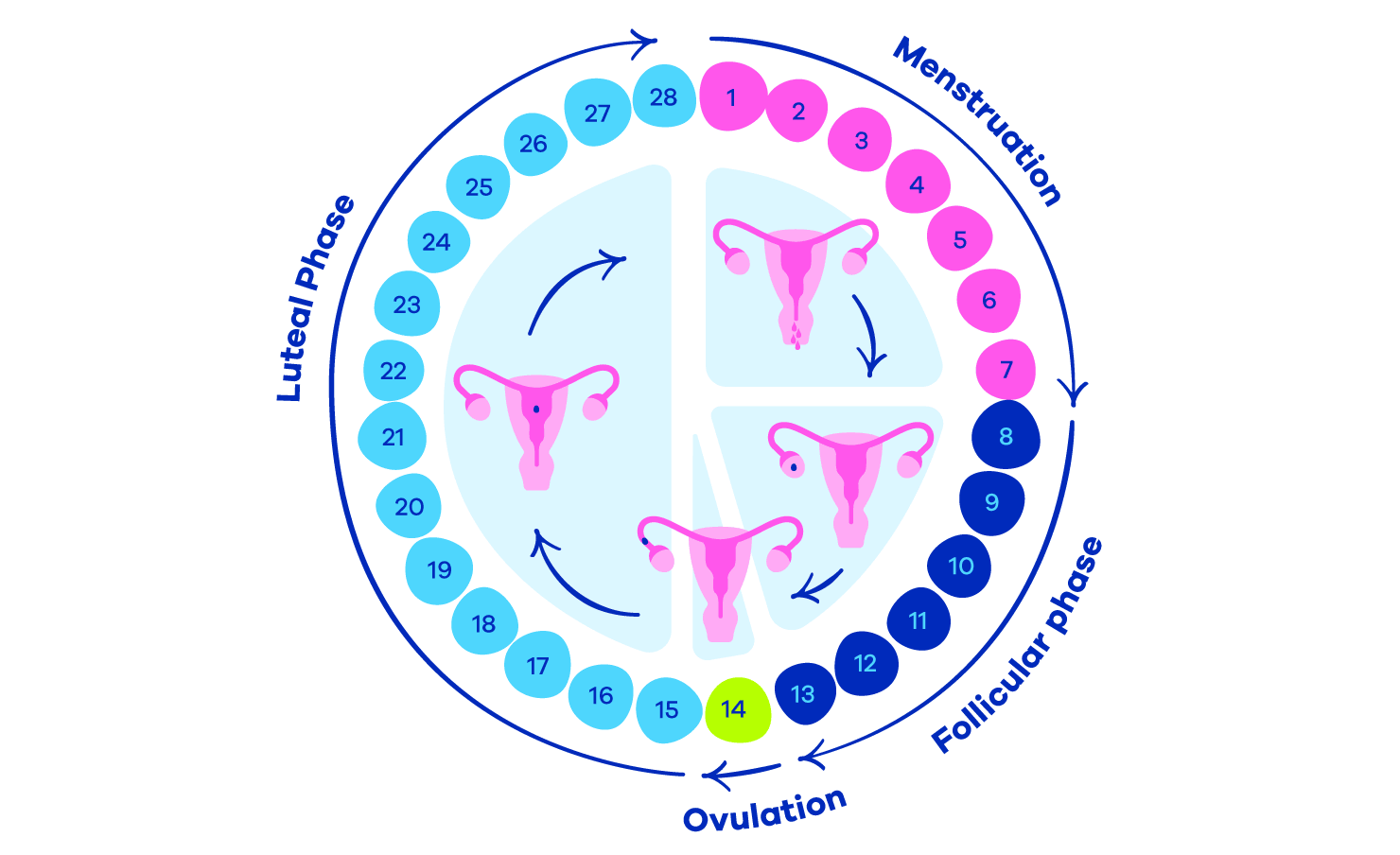
Cycle patterns, symptoms and when to seek helpThe menstrual cycle is a key window into hormonal health. Regular cycles typically fall between 21 and 35 days, but individual variation is common. What matters most is consistency and the overall pattern: sudden changes in length, volume, or pain should prompt evaluation. Heavy bleeding, prolonged periods or very painful menses can signal underlying conditions such as fibroids, endometriosis or clotting disorders that benefit from early diagnosis.
Practical self-care — tracking cycles, managing cramps with heat or appropriate analgesia, and addressing lifestyle factors such as sleep and stress — often improves day-to-day functioning. When symptoms interfere with daily life or fertility plans, a targeted clinical assessment lets clinicians personalise treatment and protect long-term reproductive health.

PCOS: Signs, Diagnosis and Management
A common, treatable hormonal conditionPolycystic ovary syndrome (PCOS) affects many women of reproductive age and presents with irregular periods, acne, excess hair growth, and sometimes difficulty conceiving. Diagnosis relies on a clinical history, examination and selected tests to assess ovulation, androgen levels and metabolic status. Because PCOS is associated with insulin resistance, addressing metabolic health is central to care.
Management focuses on individualized goals — symptom control, cycle regulation, metabolic risk reduction, and fertility when desired. Lifestyle measures (weight management, exercise, low-glycaemic nutrition) often form the first line, supplemented by hormonal therapies or insulin-sensitising medications where indicated. Regular follow-up prevents long-term complications such as diabetes and cardiovascular risk.
Fertility: Planning and Early Assessment
When to seek help and what to expectFertility depends on age, ovarian reserve, tubal and uterine health, and partner factors. Couples who have not conceived after 12 months of regular unprotected intercourse (or 6 months if the woman is over 35) should consider evaluation. Early assessment can uncover ovulatory disorders, tubal blockages, uterine factors or male infertility, allowing targeted and often successful interventions.
Preconception counselling optimises health before pregnancy — addressing nutrition, vaccination status, chronic condition control and medication review. Where needed, assisted reproductive technologies such as ovulation induction, IUI or IVF provide effective options, and emotional support throughout the process improves outcomes for many couples.
Contraception: Choosing the Right Method
Effectiveness, side effects and personal preferencesContraceptive choices should be individualised — balancing efficacy, convenience, side-effect profile and reproductive plans. Options range from barrier methods, combined or progestin-only pills, implants, IUDs (hormonal and copper), to sterilisation. Each method has advantages and limitations and suitability depends on medical history, age and lifestyle.
Discussing contraception with a clinician ensures safe selection, correct use, and management of any adverse effects. Where pregnancy is planned in the future, reversible long-acting methods provide reliable contraception without compromising later fertility when removed.

Pregnancy & Antenatal Care
Early care, risk assessment and healthy pregnancy habitsEarly antenatal care identifies risk factors, confirms gestational dating and outlines screening for conditions such as gestational diabetes, hypertension and fetal anomalies. Routine visits monitor maternal and fetal wellbeing, guide nutrition and supplementation (notably folic acid and iron), and offer vaccinations where appropriate.
Good antenatal practice emphasises balanced nutrition, appropriate weight gain, safe exercise and timely management of complications. A structured birth plan and discussion of postpartum needs help families prepare practically and emotionally for the transition to parenthood.

Mental Health and Hormonal Wellbeing
Mood, anxiety and the influence of hormonesWomen experience distinct mental-health challenges across the life-course — PMS and PMDD, perinatal mood disorders, menopausal mood changes and chronic anxiety or depression. Hormonal fluctuations can influence neurotransmitter systems and sleep, which in turn modify mood and cognitive function. Recognising these patterns allows timely support and effective treatment.
Management blends psychological therapies, social support, lifestyle measures (sleep, activity, nutrition) and pharmacotherapy when necessary. Perinatal mental health deserves special attention: prompt assessment and treatment protect both mother and child and improve long-term maternal wellbeing.

Screening and Preventive Care
Pap smears, HPV vaccination and breast healthPreventive screenings save lives. Cervical screening (Pap/HPV testing) detects precancerous changes early, and HPV vaccination prevents the strains most likely to cause cervical cancer. Regular breast awareness, clinical breast exams and appropriate imaging (mammography or ultrasound by age and risk) identify malignancies at treatable stages.
Routine health checks also include blood pressure, lipid and glucose monitoring, bone health assessment when indicated, and counselling on lifestyle risks. Building a preventive plan with a trusted clinician reduces long-term disease burden and preserves quality of life.

Menopause: Transition and Symptom Management
Navigating vasomotor, urogenital and metabolic changesMenopause marks the end of ovarian function and brings symptoms ranging from hot flushes and night sweats to vaginal dryness, sleep disruption and mood shifts. The midlife transition also alters metabolic risk, increasing the importance of cardiovascular and bone health monitoring. Individual experiences vary widely.
Symptom management is personalised — lifestyle measures, non-hormonal options and menopausal hormone therapy (when appropriate and after risk assessment) can dramatically improve quality of life. Regular screening for blood pressure, lipids and bone density supports a healthy post-reproductive life.

Nutrition, Activity and Long-Term Wellness
Dietary priorities and habits that support female healthA nutrient-dense diet tailored to life stage supports hormonal balance, fertility, bone strength and metabolic health. Iron (especially during reproductive years), calcium and vitamin D, omega-3 fats and adequate protein are central. Moderation of processed foods and refined sugars reduces inflammation and supports steady energy and mood regulation.
Regular physical activity, weight-bearing exercise, and attention to sleep and stress management form a triad with nutrition that prevents chronic disease and promotes longevity. Small, consistent habits — routine screening, balanced meals, and active living — compound into meaningful health advantages across decades.